You’re experiencing a medical revolution where bioprinters precisely deposit living cells, growth factors, and bio-materials layer-by-layer to create custom bone scaffolds that match your exact anatomy. These advanced systems achieve over 90% cell viability while incorporating natural polymers like collagen with calcium phosphates, enabling direct surgical repair and faster healing than traditional grafts. The technology’s ability to print vascular networks and release growth factors transforms how your body regenerates damaged bone tissue, offering personalized solutions that’ll reshape orthopedic medicine.
The Science Behind Bioprinting Technology for Bone Regeneration

When you’re dealing with complex bone defects, bioprinting technology offers unprecedented precision through its layer-by-layer deposition of specialized bio-inks that replicate your body’s natural extracellular matrix.
These advanced techniques, including inkjet and laser-assisted methods, enable you to create scaffolds with precisely controlled mechanical properties by combining natural polymers like gelatin and collagen with synthetic materials such as polyethylene glycol.
Advanced inkjet and laser-assisted bioprinting techniques create precisely controlled scaffolds by strategically combining natural polymers with synthetic materials for optimal mechanical properties.
You’ll benefit from hierarchical porosity that enhances nutrient transport and waste removal, essential for successful bone tissue regeneration.
The technology allows direct incorporation of growth factors and bioactive substances into your scaffolds, greatly improving vascularization and osteoinduction.
Novel formulations like gelatin methacryloyl and calcium phosphate-based bio-inks guarantee optimal printability while maintaining the biological activity necessary for effective healing.
Advanced Bio-Ink Formulations Revolutionizing Bone Tissue Engineering
As bioprinting technology advances, you’ll find that sophisticated bio-ink formulations are becoming the cornerstone of successful bone tissue engineering applications. These innovative compositions combine natural polymers like gelatin, alginate, and collagen with calcium phosphates to enhance mechanical properties and osteoconductivity. You’re witnessing breakthroughs in gelatin methacryloyl (GelMA) and gellan gum formulations that maintain exceptional cell viability during printing.
| Component Type | Primary Function | Benefits |
|---|---|---|
| Natural Polymers | Biocompatibility Enhancement | Mimics extracellular matrix |
| Calcium Phosphates | Mechanical Reinforcement | Promotes osteoconductivity |
| dECM Materials | Cellular Regulation | Enriches bioactive components |
| Nanomaterials | Strength Optimization | Improves scaffold functionality |
| Lab-made Composites | Tissue Complexity | Supports cell proliferation |
Decellularized extracellular matrix integration further enriches these formulations with bioactive components, while nanomaterial incorporation strengthens scaffold functionality for superior patient outcomes.
In Situ Bioprinting: Direct Bone Repair During Surgery
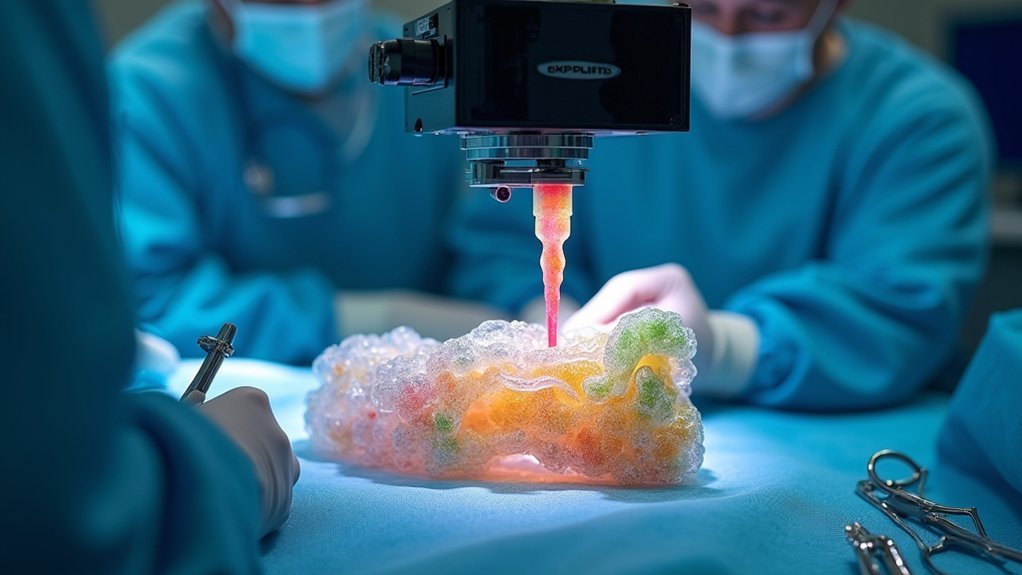
You can now repair bone defects directly during surgery using in situ bioprinting, which transforms the operating room into a real-time tissue manufacturing facility.
This approach lets you deliver customized bio-inks precisely to match each patient’s unique defect geometry while the surgical site remains open.
You’ll achieve superior healing outcomes because the printed tissue integrates immediately with surrounding bone, eliminating the complications associated with pre-fabricated implants.
Real-Time Surgical Integration
Although traditional bone grafting requires separate procedures to harvest and place materials, in situ bioprinting revolutionizes surgical repair by creating bone tissue directly within defect sites during active operations. You’ll experience immediate customization as surgeons print bio-inks precisely into your bone defect, matching its exact dimensions and conditions.
| Technology | Healing Rate | Timeline |
|---|---|---|
| Bioprinted Spheroids | 91% | 3 weeks |
| Traditional Grafting | Variable | 8-12 weeks |
| Real-time Bioprinting | 96% | 6 weeks |
| Robotic Arm Systems | Enhanced | Immediate |
| Handheld Devices | Precise | Real-time |
This real-time tissue regeneration utilizes advanced bio-inks that mimic your extracellular matrix, promoting superior cell adhesion and angiogenesis. The integration eliminates waiting periods while delivering enhanced structural integrity compared to conventional methods.
Defect-Specific Bio-Ink Delivery
The precision of real-time bioprinting reaches its pinnacle when surgeons customize bio-ink formulations to match your specific bone defect characteristics. This targeted bio-ink delivery approach tailors material composition directly to your defect’s shape, size, and biological requirements, maximizing tissue integration potential.
Advanced bioprinting techniques maintain over 90% cell viability while depositing materials precisely where you need them most. Recent spheroid-based methods demonstrate exceptional healing potential, achieving 91% tissue repair within three weeks post-surgery.
You’ll benefit from bio-inks refined for enhanced mechanical properties that match your bone’s natural strength and flexibility. This defect-specific approach eliminates the guesswork in bone defects treatment, ensuring superior tissue repair outcomes.
The precision targeting accelerates your recovery while reducing surgical complications through personalized bio-material delivery.
Enhanced Healing Outcomes
When surgeons implement in situ bioprinting during your bone repair surgery, they’re delivering living tissue directly into your defect site with unprecedented precision.
This advanced bioprinting technology transforms your healing outcomes through bio-inks that mimic your natural extracellular matrix, promoting ideal cell growth and function.
Your tissue repair benefits from remarkable achievements in bone regeneration:
- Superior cell viability – Over 90% of printed cells survive the process, ensuring robust healing
- Accelerated recovery – Printed spheroids achieve 91% healing within three weeks and 96% after six weeks
- Enhanced vascularization – Bio-inks promote angiogenesis and vascular cell migration for improved blood supply
This technology adapts to your unique defect characteristics, addressing irregular wound conditions and bleeding while enhancing integration of the printed tissue into your existing bone structure.
Patient-Specific Bone Scaffolds Through 3D Bioprinting

As surgeons face increasingly complex bone defects that vary dramatically between patients, 3D bioprinting offers an unprecedented solution for creating scaffolds tailored to each individual’s unique anatomical requirements.
You’ll find that patient-specific bone scaffolds precisely match your defect characteristics, enhancing surgical precision considerably. These scaffolds utilize biocompatible materials like natural polymers and bioactive ceramics that promote essential cell adhesion and proliferation.
The technology enables you to design scaffolds with controlled porosity and mechanical properties mimicking natural bone, facilitating ideal nutrient transport during healing.
Advanced bioprinters can incorporate growth factors directly into scaffolds, greatly boosting osteogenic properties and supporting vital vascularization.
Research consistently demonstrates that enhanced bioink formulations lead to improved healing rates in preclinical models, making personalized treatment increasingly effective.
Cellular Viability and Growth Factors in Bioprinted Bone Constructs
You’ll need to understand how cells survive the bioprinting process and continue thriving within your bone constructs.
Growth factors like BMP-2 can be strategically incorporated into your bio-inks to drive osteogenic differentiation and accelerate bone formation.
You must also implement reliable viability assessment methods to monitor cell health throughout the printing process and subsequent tissue development phases.
Cell Survival Mechanisms
Although bioprinting technology has advanced considerably, the survival of cells within printed bone constructs remains the ultimate determinant of regenerative success.
You’ll find that different printing methods achieve varying cell survival rates, with laser-assisted techniques exceeding 95% viability compared to inkjet bioprinting’s 85%.
Your choice of bio-inks directly impacts cellular survival through several mechanisms:
- Biomimetic environment creation – Natural polymers like gelatin and collagen replicate the extracellular matrix, supporting cellular attachment and function
- Optimized nutrient transport – Proper pore size and microstructure facilitate metabolic exchange within bioprinted scaffolds
- Growth factor integration – Strategic incorporation enhances cellular proliferation and differentiation for effective tissue regeneration
You must balance mechanical properties with biological functionality when optimizing bio-ink formulations to maximize survival outcomes.
Growth Factor Integration
Success in bioprinted bone regeneration hinges on your ability to strategically integrate growth factors that orchestrate cellular behavior and tissue development.
When you incorporate vascular endothelial growth factor (VEGF) into bioprinted scaffolds, you’ll enhance angiogenesis and improve nutrient delivery to developing tissue.
You’ll find that osteogenic growth factors like bone morphogenetic proteins notably boost cellular proliferation and accelerate bone tissue formation.
Maintaining over 90% cell viability during printing guarantees your cells remain responsive to these biochemical signals.
You can leverage microRNA technology for programmed differentiation, directing cells toward specific bone lineages.
Viability Assessment Methods
When evaluating bioprinted constructs, you’ll need robust assessment methods that accurately measure both cellular viability and growth factor effectiveness throughout the tissue engineering process.
Live/dead staining represents your primary tool for visualizing cellular health, displaying live cells in green and dead cells in red to assess bioprinting success.
Advanced bioprinting techniques maintain over 90% cell viability, demonstrating their effectiveness for tissue engineering applications.
You must evaluate several critical parameters:
- Growth factor release kinetics – Monitor controlled release patterns for sustained cellular signaling
- Mechanical properties assessment – Verify structural integrity supports cellular attachment and proliferation
- Cell proliferation monitoring – Track growth factor integration effects on bone morphogenetic protein activity
These thorough viability assessment methods confirm your bioprinted bone constructs achieve ideal regenerative outcomes.
Crosslinking Methods for Enhanced Bone Tissue Stability
Crosslinking methods play a pivotal role in determining the structural integrity and biological performance of bioprinted bone scaffolds.
You’ll encounter two primary approaches when selecting crosslinking methods for your bio-inks: chemical and physical crosslinking.
Chemical crosslinking uses agents like glutaraldehyde or genipin to form covalent bonds, greatly improving mechanical properties but potentially affecting cell viability if concentrations aren’t refined.
Physical crosslinking, particularly ionic gelation, offers simpler processing while preserving cell survival rates—crucial for successful bone tissue engineering applications.
Your choice directly impacts scaffold stability, pore structure, and degradation rates, all essential for nutrient transport during regeneration.
You must carefully balance crosslinking parameters, including concentration and exposure time, to achieve ideal structural integrity without compromising bioactivity in your bone tissue engineering projects.
Speed and Precision: Next-Generation Bioprinting Techniques
You’ll find that modern bioprinting has transformed bone tissue regeneration through breakthrough technologies that dramatically increase both speed and accuracy.
HITS-Bio technology now lets you fabricate tissues up to ten times faster than traditional methods while maintaining over 90% cell viability, making real-time surgical applications achievable.
When you combine this with robotic arm precision systems, you’re able to create custom bone scaffolds that perfectly match your patient’s anatomical defects with unprecedented structural integrity.
HITS-Bio Revolutionary Speed
While traditional bioprinting methods have long struggled with the trade-off between speed and cell survival, HITS-Bio shatters this limitation by delivering tissue fabrication at ten times the conventional rate without compromising cellular integrity.
You’ll witness revolutionary bone tissue regeneration capabilities that maintain over 90% cell viability throughout the process.
This breakthrough technology transforms how you approach complex tissue architectures through:
- Rapid fabrication: You can create one-cubic centimeter cartilage structures in under 40 minutes
- Simultaneous manipulation: Multiple spheroids are processed using advanced nozzle arrays for precision control
- Enhanced differentiation: MicroRNA technology programs spheroids for peak bone formation
You’ll achieve remarkable healing rates of 91% after three weeks and 96% after six weeks, making HITS-Bio the definitive solution for accelerated tissue regeneration.
Robotic Precision Applications
As robotic arm bioprinting transforms tissue engineering, you’ll experience unprecedented structural integrity and precision that surpasses traditional handheld devices in creating bone, cartilage, and skin constructs.
This bioprinting technology adapts to real-time surgical conditions, eliminating shape mismatches and adhesion problems you’d encounter with conventional methods.
You’ll benefit from robotic precision that maintains over 90% cell viability during tissue creation processes. The technology enables you to fabricate complex geometries with consistent accuracy, producing one-cubic centimeter cartilage structures in under 40 minutes.
Current research expansions focus on incorporating vascularization features into your bioprinted constructs, enhancing their functionality for regenerative applications.
You’ll soon access larger nozzle arrays capable of producing more intricate tissues, revolutionizing how you approach bone tissue regeneration in clinical settings.
Integration With Natural Bone Architecture and Vascularization
Because bone regeneration depends on recreating the complex microenvironment of natural bone, bioprinters must integrate sophisticated architectural features that support both structural integrity and biological function.
Successful bone regeneration requires bioprinters to replicate nature’s complex architectural blueprint, balancing structural durability with essential biological functionality.
When you’re developing scaffolds through bioprinting, you’re fundamentally building a foundation that mimics natural bone’s hierarchical porosity, enabling essential nutrient transport and waste removal.
Your bioprinting approach should incorporate these critical elements:
- Bioactive substances and growth factors that promote vascularization throughout the scaffold structure
- Calcium phosphates in advanced bioinks that enhance both mechanical strength and bioactivity
- Customized scaffold designs tailored to each patient’s unique anatomical requirements
This integration allows your bioprinted scaffolds to achieve remarkable healing outcomes.
Studies show that properly designed bioprinted bone grafts can deliver up to 96% healing rates in bone defects, demonstrating how effective vascularization and architectural mimicry drive successful bone regeneration.
Clinical Applications and Success Rates in Bone Defect Repair
When surgeons implement in situ 3D bioprinting techniques in actual clinical settings, they’re achieving remarkable healing outcomes that validate years of laboratory research. You’ll see healing rates reaching 91% after three weeks and 96% after six weeks when using spheroids programmed specifically for bone tissue engineering applications.
| Technology | Healing Rate | Timeframe |
|---|---|---|
| In Situ Bioprinting | 91% | 3 weeks |
| Spheroid Programming | 96% | 6 weeks |
| HITS-Bio Technique | 90% viability | 40 minutes |
Clinical applications benefit from precisely tailored scaffolds that match your individual defect conditions during surgery. The HITS-Bio technique creates cartilage structures while maintaining exceptional cell viability. Advanced bio-ink formulations enhance biocompatibility and mechanical properties, while ongoing vascularization research promises even better bone regeneration outcomes through improved blood supply integration.
Overcoming Traditional Bone Graft Limitations With Bioprinting
While traditional bone grafts have long served as the clinical standard, they’re riddled with complications that bioprinting technology now addresses head-on.
You’re no longer limited by donor site availability or concerned about immune rejection when bioprinting creates customized scaffolds.
Bioprinting transforms bone regeneration by offering:
Bioprinting revolutionizes bone healing through precise customization, enhanced regeneration, and optimized performance that traditional grafts simply cannot match.
- Precise customization – scaffolds match your exact defect dimensions
- Enhanced healing – bioactive substances and growth factors integrate directly into prints
- Optimized performance – mechanical properties align with natural bone healing
You’ll benefit from scaffolds engineered with varying degradation rates that support your body’s healing timeline.
The technology incorporates growth factors directly during printing, considerably boosting osteogenesis compared to traditional grafts.
With preclinical studies showing 96% healing rates after six weeks, bioprinting eliminates traditional limitations while accelerating regeneration.
Future Developments in Automated Bone Tissue Fabrication
As automated bioprinting evolves, you’ll witness revolutionary changes that transform how bioprinters create complex bone structures.
Future bioprinting technologies will integrate hybrid methods, combining multiple printing techniques to enhance precision and structural integrity. You’ll see automated fabrication systems incorporating vascular networks within printed constructs, greatly improving nutrient delivery and tissue health.
Expanded nozzle arrays will enable simultaneous manipulation of multiple spheroids, accelerating complex tissue architecture creation.
Advanced bioink formulations using decellularized extracellular matrices and smart materials will optimize biocompatibility and mechanical properties essential for effective bone regeneration.
Most notably, AI-driven adaptive control systems will revolutionize your printing experience by optimizing parameters in real-time, ensuring unprecedented accuracy and adaptability in automated bone tissue fabrication processes.
Frequently Asked Questions
What Is the Significance of 3D Bioprinting in Regenerative Medicine?
You’ll find 3D bioprinting revolutionizes regenerative medicine by creating precise tissue architectures with customizable bioinks that mimic natural environments. It’s achieving over 90% cell viability and 91% healing rates in surgical applications.
How Does Bone Tissue Regenerate?
Your bone regenerates through three phases: you’ll experience inflammation where clots form, then reparative callus development, and finally remodeling where mature bone replaces the callus through osteoblast and osteoclast activity.
How Do Bioprinters Work?
You’ll find bioprinters deposit bio-inks containing living cells and biomaterials in precise layers. They use inkjet, direct-write, or laser techniques with robotic control systems, then apply crosslinking methods to stabilize the printed structures.
What Are the Advantages of 3D Printing Bones?
You’ll get perfectly customized bone scaffolds that match your exact anatomy, reducing rejection risks. They incorporate growth factors for faster healing, create ideal pore structures for nutrient flow, and combine materials for superior strength.





Leave a Reply